Hip Replacement
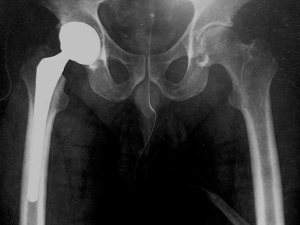 Total hip replacement (also known as total hip arthroplasty) is a surgical procedure that replaces a worn native hip joint with a metal implant with the aim to provide pain relief and restoration of function. To ensure successful surgery this procedure is best done by an orthopaedic hip surgeon.
Total hip replacement (also known as total hip arthroplasty) is a surgical procedure that replaces a worn native hip joint with a metal implant with the aim to provide pain relief and restoration of function. To ensure successful surgery this procedure is best done by an orthopaedic hip surgeon.
The reasons for the hip joint to become degenerate are multiple. The most common cause is osteoarthritis. Other causes include childhood hip disorders, fractures around the hip, avascular necrosis (loss of blood supply), infection, increased stress (overuse, overweight), inflammation such as rheumatoid arthritis.
The reason to replace a worn joint is pain that is causing considerable disability to a patient. The level of disability is highly variable among patients. Some patients require hip replacement because they cannot work and some because they are unable to do their leisure activities such as playing golf. Others choose to wait until their pain and disability interfere with walking and the activities of daily living. The decision to proceed to hip replacement is subjective and very personal. I am a specialist orthopaedic hip surgeon and I will discuss with you the benefits of surgery but also the risks associated with a hip replacement. I always advise patients to take plenty of time to think it over. Talk to your family and your local doctor about it. Feel free to ask me any questions you can think of. The patients are the ones deciding when the right time to proceed with surgery is.
Once a decision to proceed with surgery has been made I will discuss with you the surgical options that are likely to provide the best outcomes. Amongst other things, surgical options include surgical approach and hip implants.
A total hip replacement can be performed using different surgical approaches: posterior hip replacement, anterior hip replacement or anterolateral hip replacement. None of these approaches are new. The decision on which approach to use is taken after consideration of a multitude of factors such as: patient size and weight, patient skeletal anatomy, type of hip (femoral) implant to be used, other medical comorbidities.
The hip implants include acetabular components that are fixed into the pelvis and femoral components that are fixed into the femur (thigh bone). The acetabular component comprises a shell and a liner. The shell is made of titanium and usually has a hydroxyapatite coating. This shell is press fit into the bone and bone grows onto the hydroxyapatite coating. The liner is made either of polyethylene or ceramic. Another option is to use a polyethylene shell that connects to the pelvis with polymethylmetacrylate bone cement.
The femoral component comprises a stem that is connected to a ball. The stem is inserted into the femur and the fixation can be achieved using polymethylmetacrylate bone cement or the fixation can be cementless. A stem that uses cement for fixation is made of polished stainless steel whereas a cementless stem is usually made from titanium alloy with hydroxyapatite coating. The ball is usually ceramic but sometimes a metal ball is used.
The goals of surgical approach and implant selection are life long implant survival while minimizing the risk of adverse outcomes and maximizing functional performance.
I am a fellowship trained orthopaedic hip surgeon and I will provide you with the all the information required to make an informed decision. I will discuss with you my recommended surgical option that will enable the best possible outcome.

